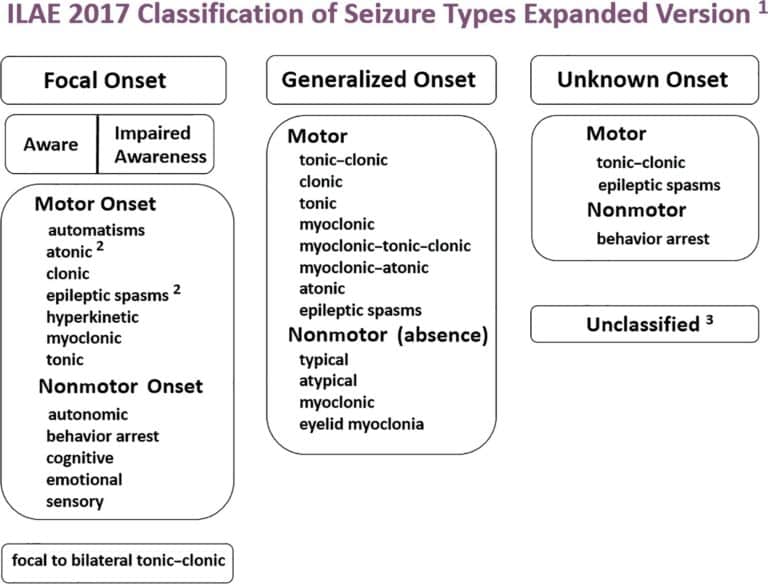
Operational classification of seizure types by the International League Against Epilepsy: Position Paper of the ILAE Commission for Classification and Terminology
Epilepsia, Volume: 58, Issue: 4, Pages: 522-530, First published: 08 March 2017, DOI: (10.1111/epi.13670)
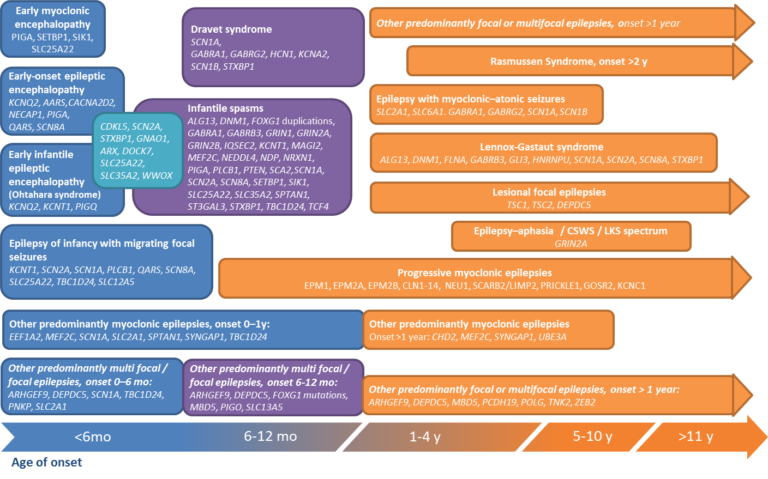
Epilepsy is not “a single disease”. With careful observation and description of the clinical manifestations (epileptic seizures and other neurological/somatin symptoms) combined to an optimal use of diagnostic tools, an increasing number of individual diseases and syndromes have emerged. Age at onset is highly variable.
In addition to a thorough clinical examination and detailed history taking, the investigational tools include video-electroencephalography and advanced neuro-diagnostics including: high resolution MRI often combined to functional neuro-imaging, genetic screening, advanced metabolic diagnostics and a neuro-psychological evaluation.

Methodology for classification and definition of epilepsy syndromes with list of syndromes: Report of the ILAE Task Force on Nosology and Definitions
Epilepsia, Volume: 63, Issue: 6, Pages: 1333-1348, First published: 03 May 2022, DOI: (10.1111/epi.17237)
EpiCARE is dealing with more than 160 rare forms of epilepsy, a number steadily augmenting as new forms of genetic epilepsies are identified every year. To those should be added the highly complex cases of focal epilepsies that could benefit from a surgical treatment. This treatment option can be proposed to patients concerned only after a long pre-surgical evaluation process assessing eligibility to a surgical treatment, an evaluation that can only be performed by multidisciplinary medical and surgical hospital-based teams. Early screening and, whenever possible, early diagnosis and the choice of the most appropriate treatments (medical or surgical) are of utmost importance.
You will find below a list of most of the rare and complex syndromes and diseases with epilepsy the ERN EpiCARE is working on.
| Related Rare or Complex Disease(s), Condition(s) | |
|---|---|
| Genetic epilepsies | • 15q13.3 microdeletion syndrome • 1p36 deletion syndrome epilepsy • Alternating Hemiplegia of Childhood (ATP1A3) • Angelman syndrome • CDKL5 (Cyclin-dependent kinase-like) deficiency disorder • Down syndrome related epilepsy • Dravet syndrome (SCN1A) • FOXG1 related epilepsies • Fragile X related epilepsy • GRIN2A related epilepsies • GRIN2B • Inversion-duplication chromosome 15q11 • KCNQ2 related epilepsies • KCNT1 related epilepsies • Pallister-Killian syndrome related epilepsy • Progressive Myoclonic Epilepsies • Protocadherin-19 (PCDH19) related epilepsy • Rett syndrome (MECP2) • Ring Chromosome 14 • Ring Chromosome 20 • SCN1A related epilepsies (other than Dravet Sd) • SCN8A related epilepsies • SYNGAP1 related epilepsies • Genetic epilepsy not otherwise identified |
| Structural epilepsies | • Angiocentric Glioma (ANET) • Arteriovenous malformation • Astrocytoma Variants • Cerebellar hamartoma • Cerebral Angioma with epilepsy • Dysembryoplastic Neuroepithelial Tumor (DNET) • Focal Cortical dysplasias • Ganglioglioma (GG) • Hemimegalencephaly • Hippocampal Sclerosis • Hypothalamic Hamartoma • Incontinentia Pigmenti • Ito Hypomelanosis • Lissencephaly • Neurofibromatosis type 1 • Periventricular Nodular Heterotopia • Polymicrogyria • Stroke (Haemorrhagic) • Stroke (Ischemic) • Sturge Weber syndrome • Subcortical band heterotopias • Tuberous sclerosis Complex • Lesional (Structural) epilepsy not otherwise identified |
| Infectious epilepsies | • Herpes simplex encephalitis • CMV encephalitis • Other Infectious-related encephalitis with epilepsy |
| Immune epilepsies | • Acute Febrile Epileptic Encephalopathy • Anti-NMDA receptor limbic encephalitis • Autoimmune encephalitis • Febrile Infection-Related Epilepsy Syndrome (FIRES) • GABA-A receptor antibody mediated immune epilepsy • GABA-B receptor antibody mediated immune epilepsy • GAD- antibody mediated immune epilepsy • Glycine receptor antibody mediated immune epilepsy • MOG-antibody mediated immune epilepsy • NORSE • Rasmussen encephalitis • Non-specified antibody related immune epilepsy • Other antibody related immune epilepsies |
| Surgically treatable epilepsies, subject to a pre-surgical evaluation | • Focal cortical dysplasias • Hypothalamic Hamartoma • Hemimegalancephaly • Low-grade developmental and epilepsy associated brain tumors (LEAT) • Cerebral cavernous malformations • MTLE with hippocampal sclerosis • Sturge-Weber syndrome • Other lesional (structural) epilepsies |
| Syndromic epilepsies | • Self-Limited Neonatal and Infantile Epilepsies • Developmental and Epileptic Encephalopathy with Spike-Wave Activation in Sleep (D/EE-SWAS) • Drug-Resistant Adolescent Absence Epilepsy • Drug-resistant Childhood Absence Epilepsy • Drug-resistant Juvenile Myoclonic Epilepsy • Early-infantile Developmental and Epileptic Encephalopathy • Epilepsy of Infancy with Migrating Focal Seizures • Epilepsy with Generalized Tonic-Clonic seizures only • Epilepsy with Myoclonic Absences (E-MA) • Hemiconvulsion-Hemiplegia-Epilepsy (HHE) • Infantile Spasms syndrome (West syndrome) • Landau-Kleffner syndrome • Lennox-Gastaut syndrome (LGS) • Myoclonic Atonic epilepsy (MAE) • Photosensitive Occipital Lobe Epilepsy (POLE) Epilepsy with Eyelid Myoclonia (E-EM) • Sleep-related Hypermotor Epilepsies |
| Metabolic epilepsies | • Pyridoxine dependent seizures (ALDH7A1) • Inborn Errors of Creatine Metabolism (including GAMT) • Molybdenum Cofactor Deficiency • POLG related epilepsies • Glucose transporter type 1 deficiency • Biotinidase deficiency • Mitochondrial diseases with epilepsy • Metabolic epilepsy not otherwise identified |
| Acute neonatal seizures | • Neonatal hypoxic and ischemic brain injury • Paediatric arterial ischemic stroke |
| Metabolic neonatal seizures | • Acute neonatal citrullinemia type 1 • Neonatal glycine encephalopathy • Pyridoxal phosphate-responsive seizures • Pyridoxine-dependent epilepsy |
| Syndromic neonatal seizures | • Self-Limited Neonatal Epilepsies (Familial or not) • Other Neonatal Epilepsies |
| Status epilepticus | • New-onset refractory status epilepticus (NORSE) • Acute encephalopathy with Inflammation-mediated status epilepticus • Continuous Spike-Waves during Slow Sleep • Febrile Infection-Related Epilepsy Syndrome (FIRES) • Non-Convulsive Status Epilepticus |